Implants
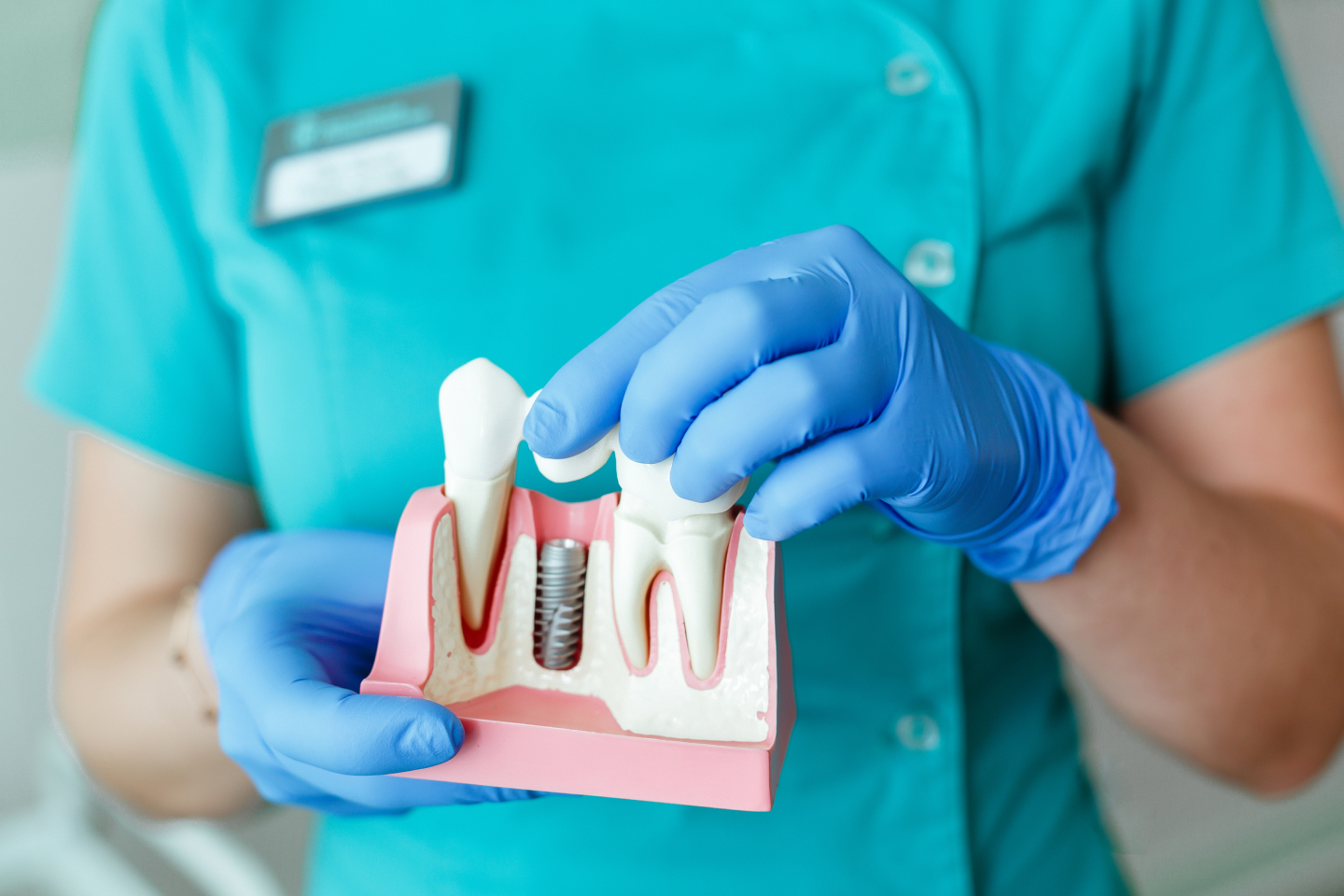
A dental implant is an artificial tooth root that is inserted into your jaw to support a bridge or prosthetic tooth. If you don't want to wear dentures and have lost one or more teeth due to periodontal disease, an accident, or another reason, dental implants may be an option for you.
Different types of Dental Implants
Endosteal (in the bone): This is the most common implant. The jawbone may be surgically implanted with screws, cylinders, or blades, among other things. One or more artificial teeth can be supported by each implant. Patients who now use removable dentures or bridges typically choose this type of implant as an alternative.
Subperiosteal (on the bone): This kind of implant is affixed to the top of the jaw using metal posts that stick out from the gum and hold the implant in place. When a patient cannot wear traditional dentures and does not have enough bone height to support an endosteal implant, subperiosteal implants are usually used.
Are Dental Implants Right for You?
A dental implant is a good choice for you if:
- Both your overall and oral health are good.
- Your jawbone is strong enough to sustain the implant.
- Your gum tissues are in good condition and free of periodontal disease.
Types of Dental Implant Procedures
Your dentist will design a treatment plan customized to your unique condition and implant type.
Single Tooth Dental Implants: If you are missing a single tooth, a single dental implant can replace it.
Multiple Tooth Dental Implants: If you are missing numerous teeth, multiple dental implants might be used to replace them.
Full Mouth Dental Implants: Full mouth dental implants can restore all of your lost teeth.
Sinus Augmentation: The quantity and quality of the bone where the implant is to be placed are important factors in implant success for sinus augmentation. Because of the lack of adequate bone, poor bone quality, and close proximity to the sinus, the upper back jaw has always been one of the hardest places to effectively insert dental implants. This issue can be resolved via sinus augmentation, which raises the sinus floor and creates bone that can support dental implants.
Ridge Modification: You may not have enough bone in your jaw to support dental implants if you have deformities in either your upper or lower jaw. To fix the issue, the gum is pulled away from the ridge to reveal the space where the bone is absent. After that, bone or a bone substitute is used to fill the space in order to create the ridge. Ridge alteration has been proven to significantly enhance the look of the jaw and raise the likelihood of successful implants.
Dental implant procedure
Step 1: Initial Assessment and Evaluation
Your dentist or oral surgeon will first do a thorough evaluation to select the most suitable dental implant technique for you based on the state of your jawbone. This preliminary examination involves X-rays, impressions, and matching the color of your teeth to ensure that your implant looks as natural as possible.
Step 2: Extraction of Teeth
If you still have a tooth that has to be replaced, your dentist will remove it before proceeding with the dental procedure. This can be done simultaneously with the implantation. Your dentist will go through your alternatives for anesthetic. Most likely, your dentist will use novocaine (or lidocaine) as a local anesthetic to numb the area and alleviate any discomfort. Unless the tooth is damaged, extraction should not take very long. During the tooth extraction, you will only feel a slight tug and pressure. Smoking, excessive spitting, blowing your nose, and drinking through a straw should all be avoided after the extraction. These actions may cause a dry socket and discomfort.
Step 3: Placing the dental implant and performing the bone graft
First, the dental implant, a small titanium post resembling a screw, is precisely positioned into the jawbone where the missing tooth once was. This process is typically performed under local anesthesia. If necessary, a bone graft may be performed. This involves adding bone material to the jaw if it lacks the necessary density or volume to support the implant. The bone graft helps stimulate new bone growth, creating a stable environment for the implant to fuse with the jawbone over time. After the procedures are completed, a healing period is required to allow the implant and bone graft to integrate before the final restoration can be attached.
Step 4: Abutment Placement
The dentist will attach an abutment to your implant once it has attained enough stability. Your crown and implant are joined together by this component. To ensure that the abutment stays in position as you eat, it must be tightened. Apart from a slight pressure, you won't experience anything throughout the procedure. Since it extends over the gum line, the abutment can sometimes be inserted at the same time as the implant.
Step 5: Adding the Permanent Crown
Your dentist will create your prosthetic tooth or crown once your gums have healed. You have the option to select either a removable implant or a permanent one. If you're getting multiple teeth at the back, similar to removable dentures, you might prefer the removable choice for the convenience of cleaning and replacement.
Having familiarized yourself with the dental implant process, it's crucial to engage in a discussion with your dentist or surgeon to address any queries and gain a comprehensive understanding of the procedure. If you're in search of a dentist specializing in dental implants and other dental services, don't hesitate to reach out to the expert team at Dental Smile-Savers in the Bronx, New York, led by Dr. Finlay. Schedule your appointment today for personalized, top-notch care.
Schedule Your Visit!
*Full Name
*Phone Number
*Comments










